Understanding molecular mechanisms of neurodegeneration
The retina is a highly specialized neural tissue that is constantly exposed to various stressors, which can compromise its function and contribute to vision-threatening diseases. Retinal stress refers to the physiological and molecular disturbances that disrupt homeostasis, leading to cellular dysfunction and degeneration. I aimed to understand the impact two such stresses namely hypoxia (caused by low oxygen) and pH stress (cause by an imbalance in pH) on the normal and the degenerating retina.
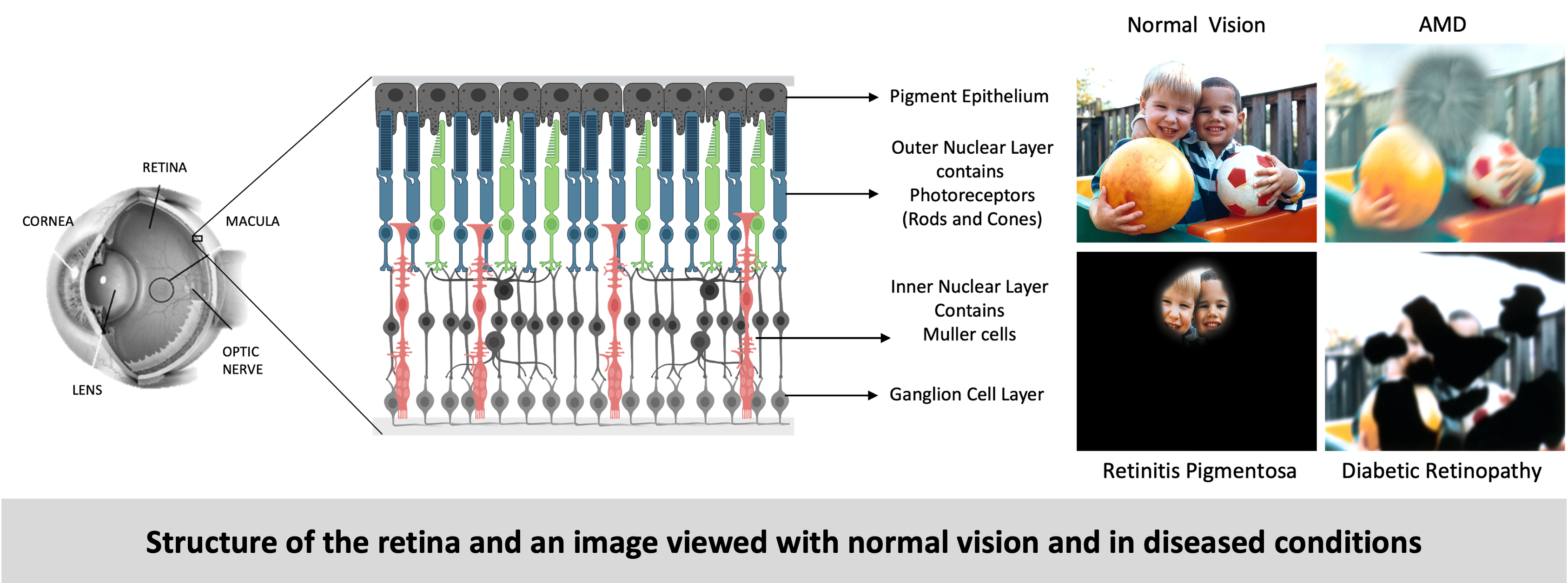
Hypoxic stress in the retina
The retina is a metabolically active tissue with high oxygen demand. Age-related changes in the retina can result in reduced oxygen supply (hypoxia) to the retina. Hypoxic stress in the retina occurs when oxygen supply is insufficient to meet the metabolic demands of retinal cells. This mild but chronic hypoxia results in cellular stress and eventual death of retinal cells leading to degeneration. At the cellular level the hypoxic response is mainly executed by transcription factors called – hypoxia inducible factors (HIFs). In this project, by using genetic mouse models, we aimed to understand the role of hypoxia pathways and more specifically HIFs in age-related retinal degeneration. So, we generated mouse models with rod photoreceptor-specific overexpression or knockdown of the transcription factors HIF1A and HIF2A. Upon characterization of these mice, we showed that overexpression of HIF1A resulted in loss of photoreceptors which led to retinal degeneration. In mice with HIF1A knockdown, this phenotype was rescued. To analyze molecular and cellular changes we compared the transcriptomes of retinas when HIF1A is overexpressed or deleted in the rods, which revealed the differential regulation of several genes. Based on the groups of differentially regulated genes identified, we focused our analysis on two important mechanisms – metabolism and immune response (complement pathway). In HIF1A stabilized mice there was an upregulation of complement factors, however upon further analysis we concluded that the complement factors are not direct targets of HIF1A and are most likely upregulated as part of ongoing degeneration mechanisms in these mice. We also showed that HIF1A stabilization resulted in a metabolic shift from oxidative phosphorylation to glycolysis. Lastly, the knockdown of Hif1a in the hypoxic retina, by subretinal injections of Adeno-associated viruses (AAVs) packaging shRNA against Hif1a was envisioned as a gene therapy for combating degeneration.
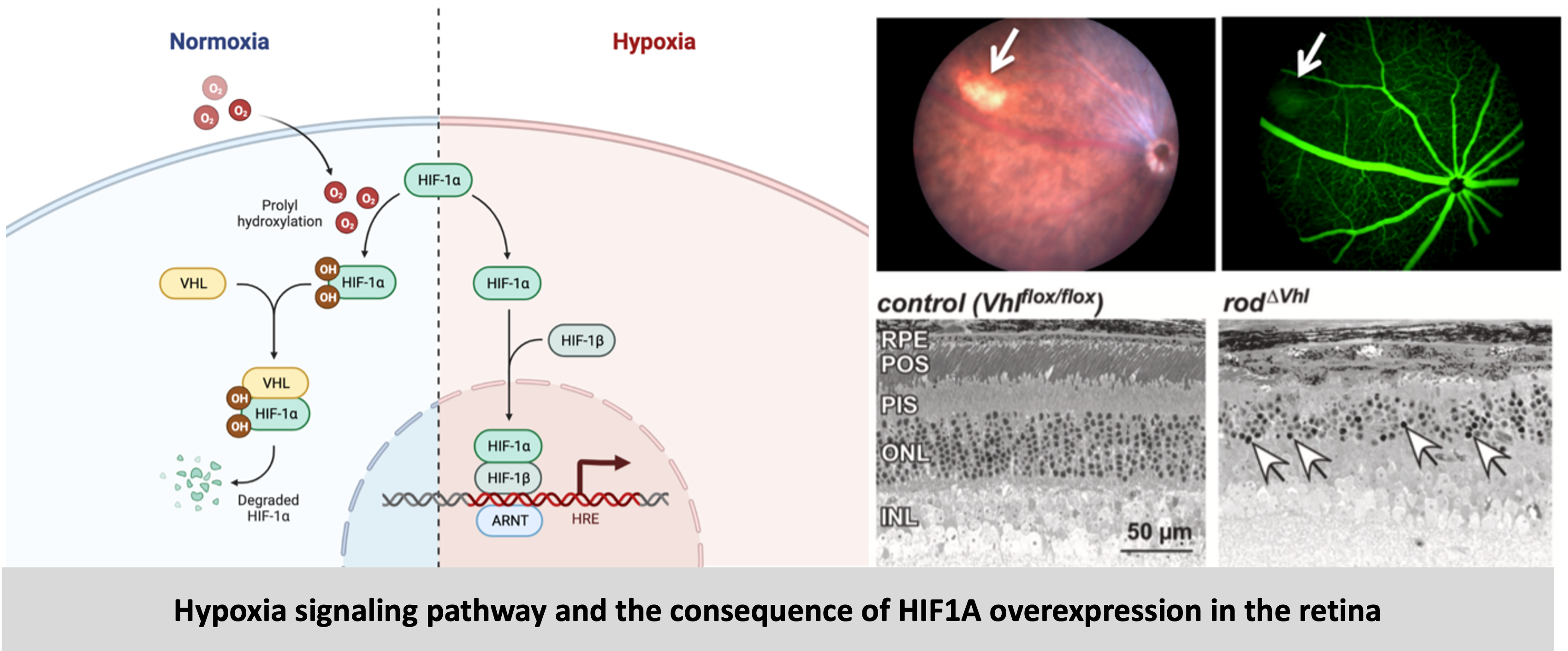
Read the details and the results of this project here
Hif1a inactivation rescues photoreceptor degeneration induced by chronic hypoxia-like stress.
Barben M*, Ail D*, Storti F, Klee K, Schori C, Samardzjia M, Michalakis S, Biel M, Meneau I, Blaser F, Barthelmes D, Grimm C
Cell Death and Differentiation, 2018
pH stress in the retina
In addition to hypoxic stress, the retina is also susceptible to other types of stress such as pH changes and the ensuing acidosis during degeneration. Hence, we analyzed a class of proton sensing G-protein coupled receptors (GPRs) – Gpr4, Gpr65 and Gpr68 in the retina. Our studies revealed that all the three GPRs are expressed in the retina, but only Gpr65 is upregulated during induced (light damage model) and inherited (rd10 mice) degeneration. Knockout mice lacking GPR65 had normal retinal structure and function, but the additional loss of Gpr65 in rd10 mice accelerated degeneration. Since GPR65 was dispensable for normal retinal development, function and aging as evidenced by the evaluation of Gpr65−/− mice, our results indicate that the proton-sensing G protein-coupled receptor GPR65 may be involved in a mechanism that supports survival of photoreceptors in the degenerating retina.
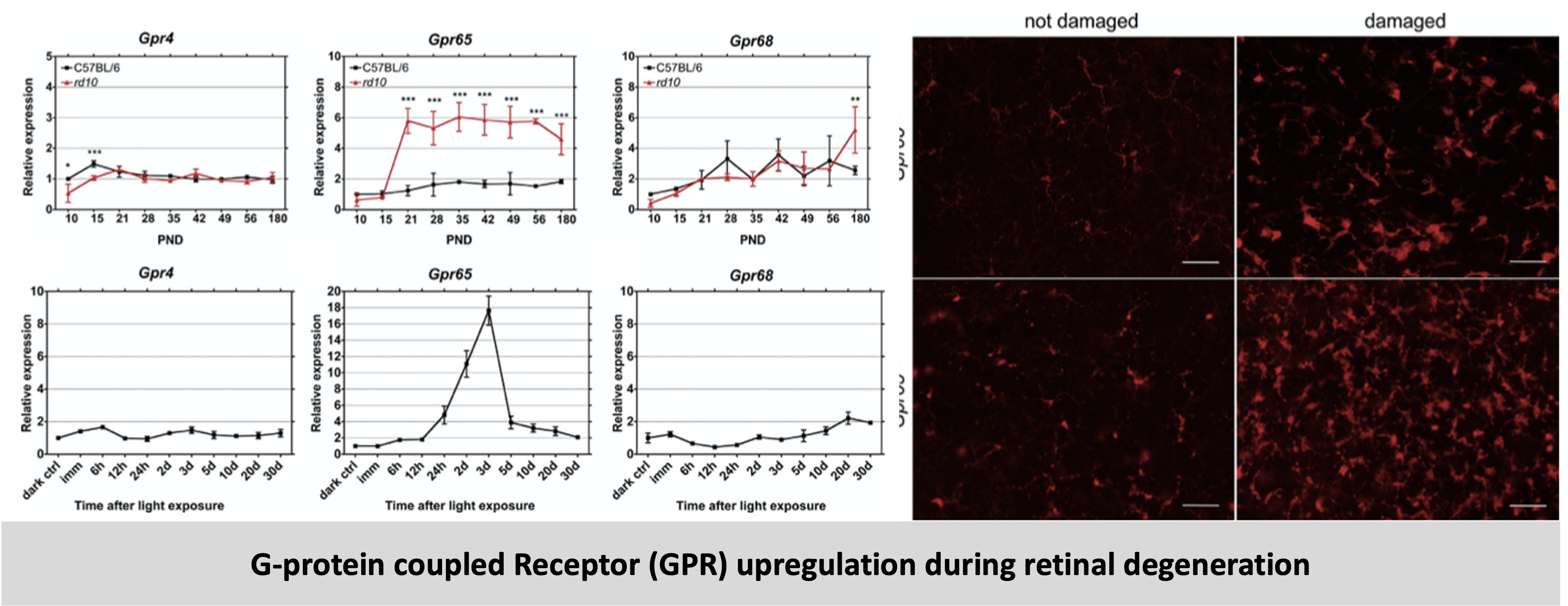
Read the details and the results of this project here
Increased expression of proton-sending G protein-coupled receptor Gpr65 during retina degeneration.
Ail D*, Rüfenacht V*, Caprara C, Samardzjia M, Grimm C
Neuroscience, 2015
The projects on hypoxia and retinal degeneration were conducted in the Lab of Retinal Cell Biology (LRCB) at the University of Zurich, Switzerland as part of my PhD thesis. The lab was mainly involved in the study of degenerative retinal diseases and my focus was on hypoxic stress and more specifically on investigating the role of the transcription factor – hypoxia inducible factor 1A (HIF1A) in retinal degeneration. My PhD work was conducted at the University of Zurich as part of the Neuroscience (ZNZ) PhD program in the Life Science Graduate School of Zurich (LSGSZ).
